Blood Pressure Stages Explained: Normal, Elevated & Hypertension
What do blood pressure stages mean? Learn the difference between normal, elevated, stage 1 and stage 2 hypertension, plus when readings become a medical emergen
What do blood pressure stages mean? Learn the difference between normal, elevated, stage 1 and stage 2 hypertension, plus when readings become a medical emergen
When your doctor mentions that your blood pressure has moved into a new stage, it sounds ominous. But the stages are not a mystery. They are categories defined by medical guidelines to help clinicians and patients understand cardiovascular risk and decide when action is needed.
The American College of Cardiology and the American Heart Association updated these stages in 2017, tightening the thresholds and reclassifying millions of Americans into higher-risk categories overnight. The goal was not to scare people. It was to intervene earlier, before damage accumulates.
If you use a home blood pressure monitor, you will see numbers. Understanding which stage those numbers fall into helps you know whether to relax, watch closely, or call your doctor today.
The five blood pressure stages
Blood pressure stages are based on two measurements: systolic (the top number, pressure when the heart beats) and diastolic (the bottom number, pressure when the heart rests). Both matter, and guidelines classify you based on whichever number is worse.
Here is the current breakdown:
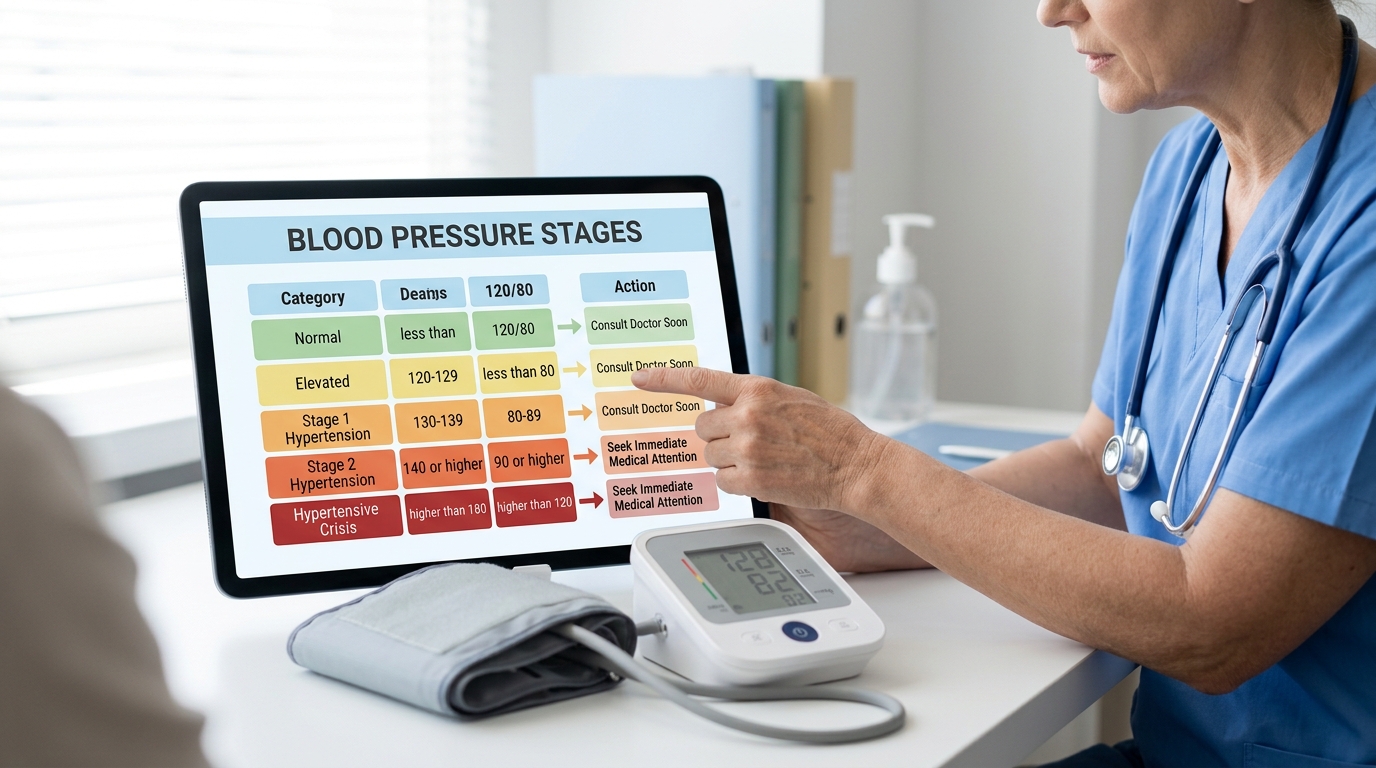
1. Normal: Less than 120/80 mmHg
This is the target. A reading below 120 systolic and below 80 diastolic means your cardiovascular system is operating within a healthy range. You do not need treatment, just routine monitoring and healthy habits to keep it there.
2. Elevated: 120–129 systolic and less than 80 diastolic
Elevated blood pressure means your systolic number has crept into the 120s, but your diastolic is still below 80. This stage does not yet qualify as hypertension, but it is a warning. Without changes, elevated blood pressure often progresses to full hypertension within a few years.
At this stage, your doctor will likely recommend lifestyle changes before considering medication: weight loss if needed, exercise, less sodium, more potassium, stress management, and limited alcohol.
3. Stage 1 Hypertension: 130–139 systolic or 80–89 diastolic
Stage 1 hypertension is diagnosed when your systolic is between 130 and 139, or your diastolic is between 80 and 89. Notice the or. If either number is in this range, you have stage 1 hypertension, even if the other number is normal.
This is where treatment discussions begin. If you have no other cardiovascular risk factors (no diabetes, no prior heart attack, no kidney disease), your doctor may still start with lifestyle changes and monitor for a few months. But if your 10-year cardiovascular risk is elevated, medication may be recommended immediately.
Stage 1 is not an emergency, but it is not something to ignore. Prolonged exposure to even mildly elevated blood pressure increases the risk of heart attack, stroke, kidney damage, and heart failure over time.
4. Stage 2 Hypertension: 140/90 mmHg or higher
Stage 2 hypertension is defined as systolic 140 or higher, or diastolic 90 or higher. At this stage, medication is almost always recommended, usually in combination with lifestyle changes.
The risk of cardiovascular events rises sharply once readings consistently reach or exceed 140/90. Even if you feel fine, this level of pressure is silently straining your heart, blood vessels, kidneys, and brain.
If you are diagnosed with stage 2 hypertension, expect to start on at least one blood pressure medication, with regular follow-up to adjust the dose or add a second drug if needed.
5. Hypertensive Crisis: Higher than 180/120 mmHg
A reading above 180 systolic or above 120 diastolic is a hypertensive crisis. This is not a stage you monitor at home and discuss at your next appointment. This is a medical emergency.
There are two types of hypertensive crisis:
- Hypertensive urgency: Blood pressure is dangerously high, but you have no symptoms of organ damage (no chest pain, shortness of breath, severe headache, vision changes, or confusion). You need immediate medical attention, but it may not require an ambulance.
- Hypertensive emergency: Blood pressure is dangerously high and you are experiencing symptoms of organ damage. Call 911 immediately.
If your monitor shows a reading above 180/120, wait a few minutes, take a second reading to confirm, and seek medical help. Do not wait to see if it comes down on its own.

Which number matters more?
Both systolic and diastolic pressure matter, but systolic pressure becomes a stronger predictor of cardiovascular risk as you age. In younger adults, diastolic pressure may be more telling. In older adults, systolic pressure tends to rise while diastolic may stay flat or even drop, a pattern called isolated systolic hypertension.
Guidelines classify you based on whichever number is worse. If your reading is 138/76, you have stage 1 hypertension, even though your diastolic is normal. If your reading is 118/88, you also have stage 1 hypertension, because the diastolic crosses the threshold.
One high reading does not define your stage
Blood pressure fluctuates. A single reading of 145/92 does not mean you have stage 2 hypertension if your usual readings are lower. Diagnosis requires multiple elevated readings taken on different days, ideally at different times of day.
This is why home blood pressure monitors are so useful. They let you build a pattern. Your doctor is not interested in one scary reading. They want to see your average over a week or two.
Why the thresholds changed in 2017
Before 2017, stage 1 hypertension was defined as 140/90 or higher. The new guidelines lowered the threshold to 130/80, reclassifying millions of people who previously had “prehypertension” into stage 1 hypertension.
The change was based on large-scale studies showing that cardiovascular risk begins to rise well before 140/90. By treating earlier, the goal is to prevent heart attacks, strokes, and kidney disease before they happen.
Critics argued that the change medicalized too many people and could lead to overtreatment. Proponents pointed out that the new guidelines still prioritize lifestyle changes and only recommend medication for people with elevated cardiovascular risk.
Either way, the current standard is 130/80. That is the threshold your doctor will use.
What to do at each stage
Normal (less than 120/80)
- Continue healthy habits.
- Recheck blood pressure at routine doctor visits, or annually at home if you have risk factors.
Elevated (120–129 and less than 80)
- Focus on lifestyle: exercise, weight loss if needed, reduce sodium, manage stress.
- Recheck every 3–6 months.
- No medication unless you have other cardiovascular risk factors.
Stage 1 Hypertension (130–139 or 80–89)
- Lifestyle changes are essential.
- Medication may be recommended if you have diabetes, kidney disease, or high cardiovascular risk.
- Recheck within 1–3 months, or sooner if starting medication.
Stage 2 Hypertension (140/90 or higher)
- Lifestyle changes plus medication, usually starting with one or two drugs.
- Close follow-up to adjust treatment as needed.
- Home monitoring strongly recommended to track response.
Hypertensive Crisis (higher than 180/120)
- Wait a few minutes and recheck.
- If still elevated, seek medical care immediately.
- If you have symptoms (chest pain, shortness of breath, severe headache, vision changes), call 911.
Home monitoring helps clarify your stage
Blood pressure varies throughout the day. A reading at a doctor’s office may be higher than your usual due to white coat effect. A reading at home after a stressful day may be higher than your morning baseline.
The most reliable way to understand your true blood pressure stage is to take multiple readings at home, ideally at the same time each day, and average them over a week or two. This gives your doctor a much clearer picture than a single office reading.
A validated, properly-sized upper-arm monitor is the gold standard for home use. If you do not have one yet, our guide to the best home blood pressure monitors walks through the models we recommend for accuracy and ease of use.
Stages are not permanent
If you are diagnosed with stage 1 or stage 2 hypertension, that does not mean you are stuck there. Many people move back down to normal or elevated ranges with medication, weight loss, exercise, and dietary changes.
Conversely, if you are currently at elevated or normal, that does not mean you will stay there. Blood pressure tends to rise with age, especially if lifestyle habits drift. Regular monitoring helps you catch changes early, when they are easiest to reverse.
The bottom line
Blood pressure stages are a tool for understanding risk and guiding treatment. Normal is the goal. Elevated is a yellow light. Stage 1 and stage 2 hypertension require action, often including medication. Hypertensive crisis requires immediate medical attention.
If you know which stage you are in, you know what to do next. And if you are monitoring at home, you have the data to see whether your current approach is working or whether it is time to adjust.
Home-monitoring advice is only useful if it is easy to verify and act on correctly.
We write explainers to be understandable to readers, search engines, and AI answer systems.
Use a validated upper-arm monitor and track readings over time, not just once.

