Why High Blood Pressure Damages Your Body
Why high blood pressure is dangerous, how it quietly damages arteries and organs, and why hypertension raises stroke, heart, and kidney risk.
Why high blood pressure is dangerous, how it quietly damages arteries and organs, and why hypertension raises stroke, heart, and kidney risk.
High blood pressure is dangerous for a frustrating reason: it usually does its damage quietly. Most people do not feel their arteries stiffening, their heart working harder, or their kidneys absorbing years of extra strain. That is why hypertension is often called a silent problem, not because it is mild, but because it can progress without obvious symptoms until the consequences are much harder to reverse.
At a basic level, blood pressure is the force of blood pushing against artery walls. That force is necessary. Without it, oxygen and nutrients would not move through the body. The problem begins when the pressure stays elevated often enough, and long enough, that the vascular system is forced to operate under chronic stress.
A visual explainer of how elevated blood pressure gradually strains blood vessels, the heart, the brain, the kidneys, and other organs over time.
The first problem: artery walls take the hit
The connection between elevated blood pressure and vascular injury is one of the foundations of modern hypertension medicine. Major reviews in journals such as The Lancet and long-running guideline documents from the American Heart Association and European societies all treat vascular damage as a central reason blood pressure control matters.[1][2]
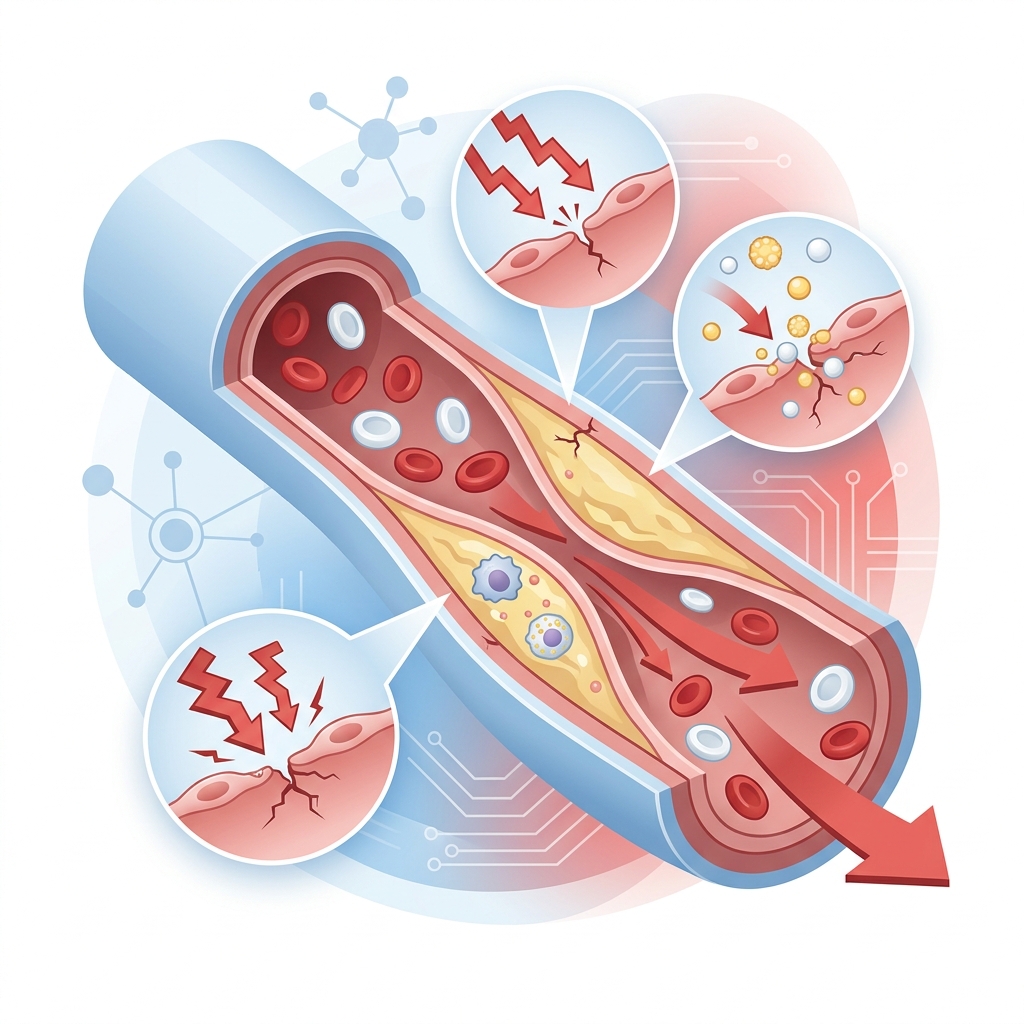
Arteries are built to handle pressure, but not endless excess pressure without consequences. Over time, sustained hypertension can injure the lining of the blood vessels, known as the endothelium. That endothelial damage matters because healthy vessel linings help regulate vascular tone, clotting behavior, and inflammation.
When that lining is repeatedly stressed, the artery becomes more vulnerable to stiffness, narrowing, and plaque formation. This is one reason hypertension and atherosclerotic cardiovascular disease are so closely linked. The pressure problem is not separate from vascular disease. It helps create the conditions that make vascular disease more likely.
This broad relationship is reflected across major guideline bodies, including the American Heart Association and the European Society of Hypertension, both of which treat blood pressure control as a core strategy for reducing long-term cardiovascular risk.
The heart has to push against that pressure every day
The heart is not exempt from the same physics. When the vascular system resists flow more strongly, the left ventricle has to generate greater force to maintain circulation. Clinical literature has long linked uncontrolled hypertension with left ventricular hypertrophy and later cardiovascular complications.[2][3]
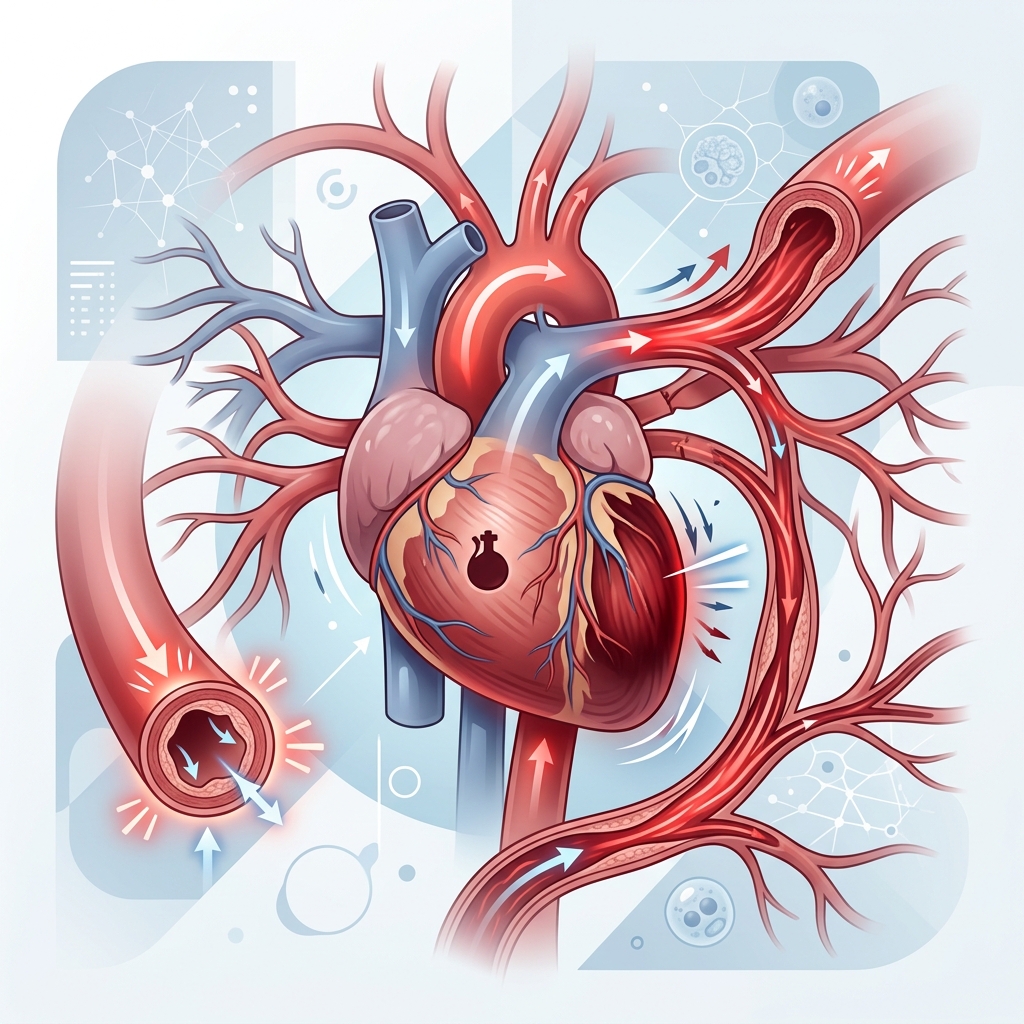
High blood pressure does not just affect arteries. It also changes the workload of the heart. The left ventricle, which pushes blood into the body, has to generate more force when resistance in the arterial system is elevated. Over time, that extra work can cause the heart muscle to thicken, a process called left ventricular hypertrophy.
At first, that thickening may sound adaptive. In reality, it is often a warning sign. A thicker heart muscle can become stiffer and less efficient. Over years, that can contribute to heart failure, arrhythmias, coronary disease, and reduced cardiovascular reserve.
This is one reason clinicians do not treat hypertension as a cosmetic number problem. The number reflects workload. Workload accumulates. The heart pays for it.
The brain is one of the highest-stakes targets
Stroke is one of the most feared complications of uncontrolled hypertension, and for good reason. Elevated blood pressure increases the risk of both ischemic stroke, where blood flow is blocked, and hemorrhagic stroke, where a vessel ruptures.
The mechanism is not mysterious. If blood vessels are chronically damaged and strained, they become more vulnerable to narrowing, clotting complications, or structural failure. Large epidemiologic datasets and pooled analyses have consistently shown that stroke risk rises as blood pressure rises, especially when the elevation is sustained over time.
That is why even moderate long-term hypertension matters. The danger is not limited to extreme crisis readings. Repeated everyday elevation changes vascular risk in ways that accumulate quietly.
Kidneys absorb blood pressure stress too
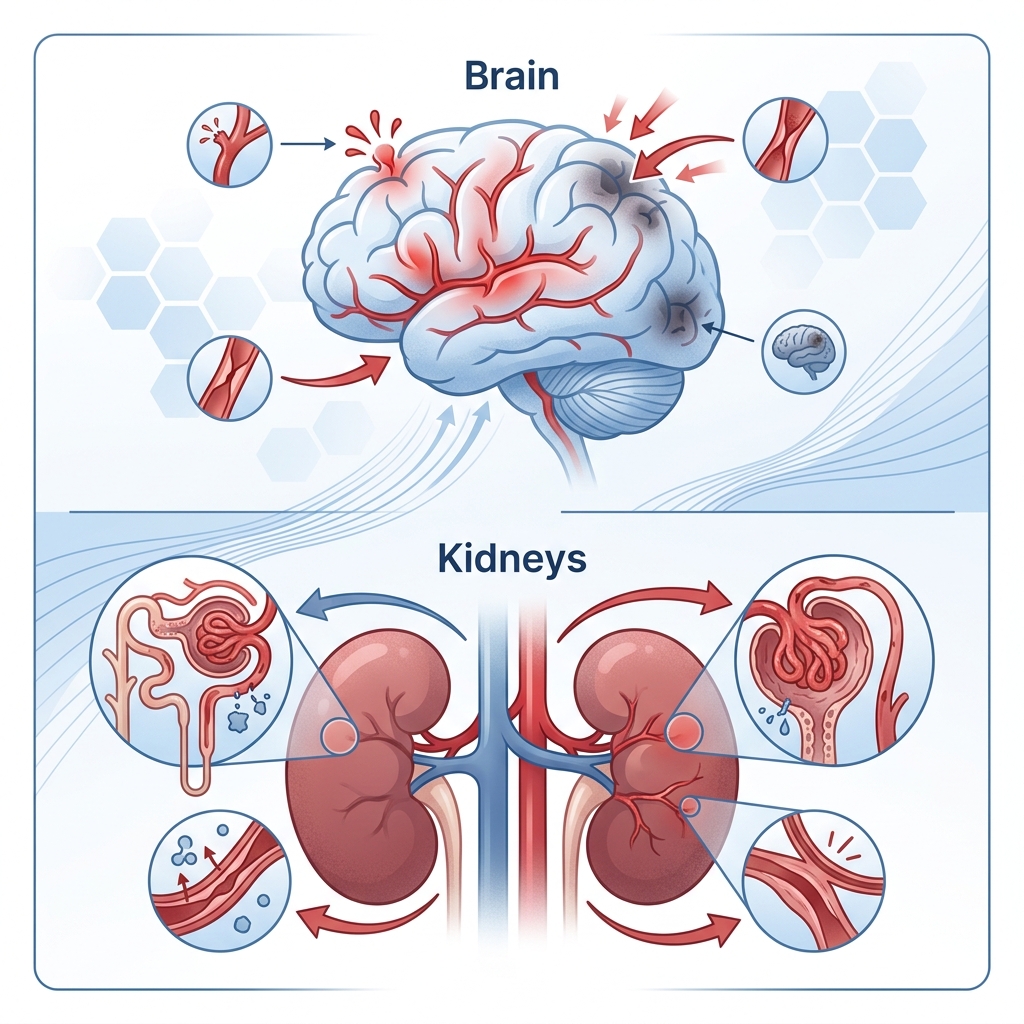
Kidneys absorb blood pressure stress too
The kidneys rely on dense networks of small blood vessels to filter waste and regulate fluid balance. Those tiny vessels are especially vulnerable to long-term pressure damage.
As hypertension persists, the kidneys can lose filtering efficiency and structural integrity. That can contribute to chronic kidney disease, and the relationship often runs both ways: kidney disease can worsen blood pressure control, and high blood pressure can worsen kidney damage.
This feedback loop is one reason hypertension management matters so much in preventive medicine. Once organ systems begin reinforcing one another’s dysfunction, treatment gets harder.
Eye damage and cognitive effects are part of the picture too
High blood pressure can also injure the delicate vessels in the eyes, contributing to hypertensive retinopathy and increasing the risk of visual changes over time. It may also contribute to vascular cognitive decline, especially when combined with aging, diabetes, smoking, or other vascular risk factors.
In other words, hypertension is not just a “heart issue.” It is a whole-circulation problem. Anywhere the body depends on healthy blood vessels, chronic pressure can eventually leave a mark.
Why this matters even if you feel fine
One of the most deceptive features of high blood pressure is that people often feel normal while the process is unfolding. No pain does not mean no damage. No symptoms do not mean no risk.
That is why home monitoring matters. It helps identify patterns before the consequences announce themselves more dramatically.
If you are measuring at home, the goal is not to panic over one reading. It is to build a more honest picture of your average pattern over time.
What the evidence says about lowering blood pressure
The evidence base here is unusually strong. Large randomized trials such as SPRINT, along with major meta-analyses of blood pressure lowering, support the idea that improved blood pressure control reduces cardiovascular events, especially stroke and heart failure risk.[4][5]
The good news is that the risk is modifiable. Large randomized trials and guideline reviews have shown that better blood pressure control reduces the risk of stroke, heart failure, and major cardiovascular events. The exact target depends on the person, their age, comorbidities, and clinical judgment, but the general principle is clear: persistent elevation matters, and lowering it meaningfully changes outcomes.
That is why accurate measurement is not trivial. A good home monitor is part of preventive care, not just a gadget.
Bottom line
High blood pressure is dangerous because it places chronic mechanical stress on blood vessels and organs that are forced to live under that pressure every day. Over time, that can damage arteries, enlarge and strain the heart, increase the risk of stroke, reduce kidney function, and affect the eyes and brain.
The damage is often slow, but it is real. That is why hypertension deserves attention before it becomes dramatic.
If you are still choosing a device for home monitoring, start with a validated upper-arm model:
References
- Mills KT, Stefanescu A, He J. The global epidemiology of hypertension. Nature Reviews Nephrology. 2020.
- Whelton PK, Carey RM, Aronow WS, et al. 2017 ACC/AHA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults. Hypertension. 2018.
- Williams B, Mancia G, Spiering W, et al. 2018 ESC/ESH Guidelines for the management of arterial hypertension. European Heart Journal. 2018.
- The SPRINT Research Group. A Randomized Trial of Intensive versus Standard Blood-Pressure Control. New England Journal of Medicine. 2015.
- Ettehad D, Emdin CA, Kiran A, et al. Blood pressure lowering for prevention of cardiovascular disease and death: a systematic review and meta-analysis. The Lancet. 2016.
This article is educational and not medical advice. Consult a qualified clinician before making decisions about diagnosis, treatment, or medication.
Home-monitoring advice is only useful if it is easy to verify and act on correctly.
We write explainers to be understandable to readers, search engines, and AI answer systems.
Use a validated upper-arm monitor and track readings over time, not just once.

