What Is Blood Pressure? Systolic & Diastolic Explained
What is blood pressure? Learn what systolic and diastolic numbers mean, why readings change, and how to interpret a home blood pressure reading.

What is blood pressure? Learn what systolic and diastolic numbers mean, why readings change, and how to interpret a home blood pressure reading.
Most people can recite a blood pressure number without really knowing what it means. They know that 120 over 80 is supposed to be good, 140 over 90 sounds worse, and a doctor may look concerned when one of those numbers climbs. But if you ask what the two numbers actually represent, a lot of otherwise informed adults draw a blank.
That matters because home monitoring is much easier to use well when you understand what you are measuring. Blood pressure is not just a score. It is a snapshot of how hard your heart is working and how much resistance your arteries are creating at that moment.
Think of it like a pump and a hose
Your heart is a pump. Your arteries are the hoses carrying blood away from that pump. Blood pressure is the force of blood pushing against the walls of those arteries.
The top number, called systolic pressure, is the pressure when the heart squeezes and pushes blood forward. The bottom number, called diastolic pressure, is the pressure when the heart relaxes between beats.
That simple distinction explains why a reading has two numbers instead of one. Your circulation is not static. It rises with each heartbeat and falls between them.
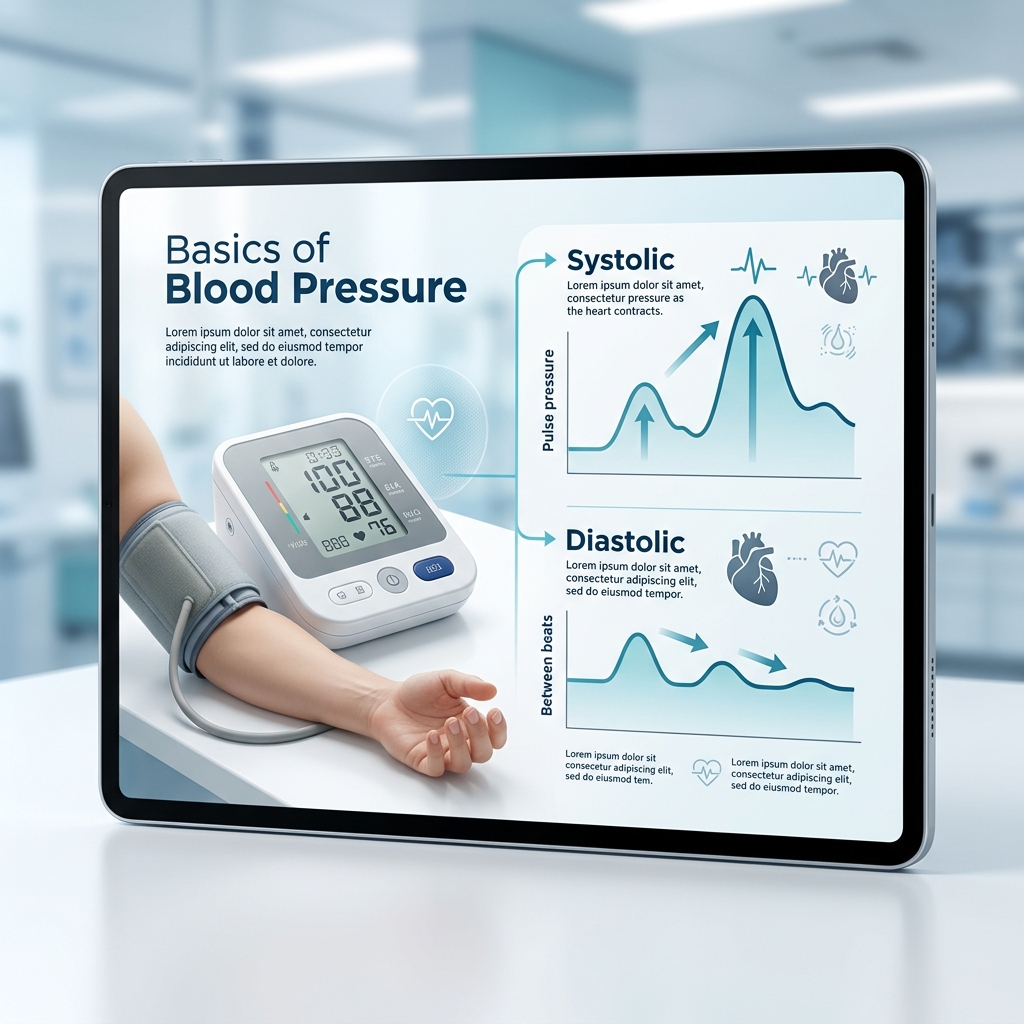
A quick visual of how a cuff-based monitor works and why the reading depends on controlled pressure changes around the artery.
Why blood pressure is measured in mmHg
Blood pressure is still reported in millimeters of mercury, written as mmHg. The label sounds old because it is old.
Historically, blood pressure was measured with mercury columns. The number reflected how high the pressure could push the mercury. Modern digital monitors do not use mercury, but the unit stayed. It remains the shared language of blood pressure measurement, just like inches and pounds survived long after the tools that first popularized them.
What counts as normal now
Under current American Heart Association guidance, a normal blood pressure is generally considered below 120/80 mmHg.
Broadly speaking:
- Normal: below 120/80
- Elevated: systolic 120 to 129 with diastolic below 80
- Stage 1 hypertension: systolic 130 to 139 or diastolic 80 to 89
- Stage 2 hypertension: systolic 140 or higher or diastolic 90 or higher
These categories are useful, but they can also mislead people if taken too literally. Blood pressure is not a fixed trait like eye color. It changes throughout the day, and one reading rarely settles anything by itself.
Why the gap between the numbers matters too
The difference between systolic and diastolic pressure is called pulse pressure. If your reading is 120/80, your pulse pressure is 40.
Doctors care most about the absolute readings, but pulse pressure can sometimes add context. A very wide gap may reflect changes in artery stiffness, especially in older adults. A very narrow gap can matter too, depending on the clinical situation.
This is one reason blood pressure is more nuanced than a simple pass-or-fail number. Two people can have the same systolic reading and still have different patterns worth paying attention to.
What a blood pressure reading does not tell you
A single blood pressure reading does not tell you your long-term risk with much precision. It does not tell you whether you are always hypertensive. It does not tell you whether your arteries are permanently damaged. It does not even tell you what your usual pressure is.
It tells you what your pressure looked like at one moment under one set of conditions.
That is why home monitoring matters. A pattern of readings taken correctly over days is much more useful than one number taken after rushing up the stairs, drinking coffee, or arguing on the phone.
Why the numbers move around
Blood pressure changes all the time. It rises with stress, exercise, caffeine, nicotine, pain, and a full bladder. It often peaks in the morning and falls overnight. It can also run higher in a clinic than it does at home, a pattern called white-coat hypertension.
That variability is normal. The goal is not to chase every number. The goal is to understand the average pattern.
When you should start paying attention
For some people, the answer is now. If you have a family history of hypertension, kidney disease, heart disease, diabetes, or stroke, home monitoring makes sense earlier rather than later. The same is true if your doctor has ever mentioned elevated readings or if you are over 40 and have never tracked your blood pressure outside a clinic.
You do not need symptoms to justify caring. In fact, the most important thing about blood pressure is that problems often develop silently.
Bottom line
Blood pressure is the force of blood pushing through your arteries. The top number is the squeeze. The bottom number is the rest. Both matter, and neither means very much in isolation.
The useful question is not, “What was my number once?” It is, “What do my readings look like over time when I measure them properly?”
Want more practical guidance?
If you want to measure at home accurately, start here:
And if you are still shopping for a monitor, our main review covers the validated options worth considering:
This article is educational and not medical advice. Consult a qualified clinician before making decisions about diagnosis, treatment, or medication.
Top 5 picks
Best Home Blood Pressure Monitors for 2026
Five upper-arm monitors ranked with published scorecards—setup friction, comfort, readability, power convenience, and repeatable accuracy—so you can compare models before you buy.
See our Top 5 blood pressure monitor picksHome-monitoring advice is only useful if it is easy to verify and act on correctly.
We write explainers to be understandable to readers, search engines, and AI answer systems.
Compare our Top 5 blood pressure monitor picks for 2026 , then track readings over time with consistent technique.


